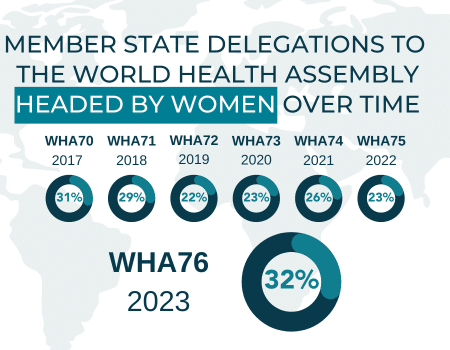
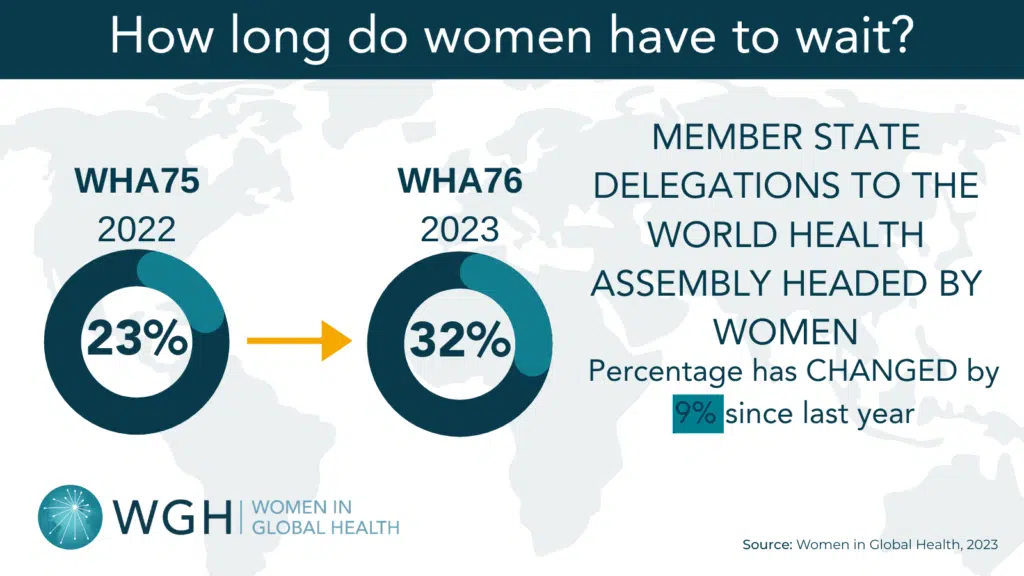
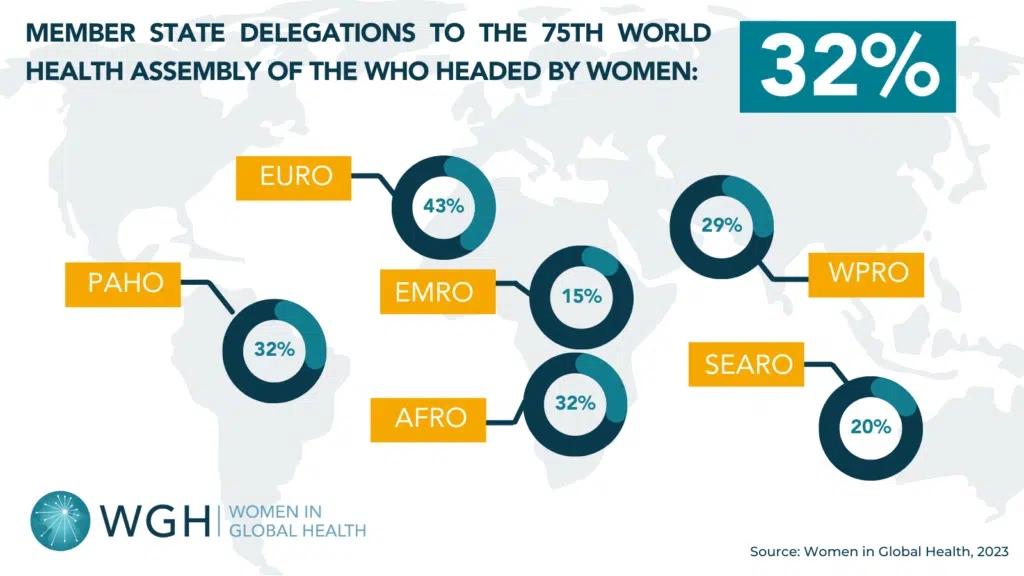
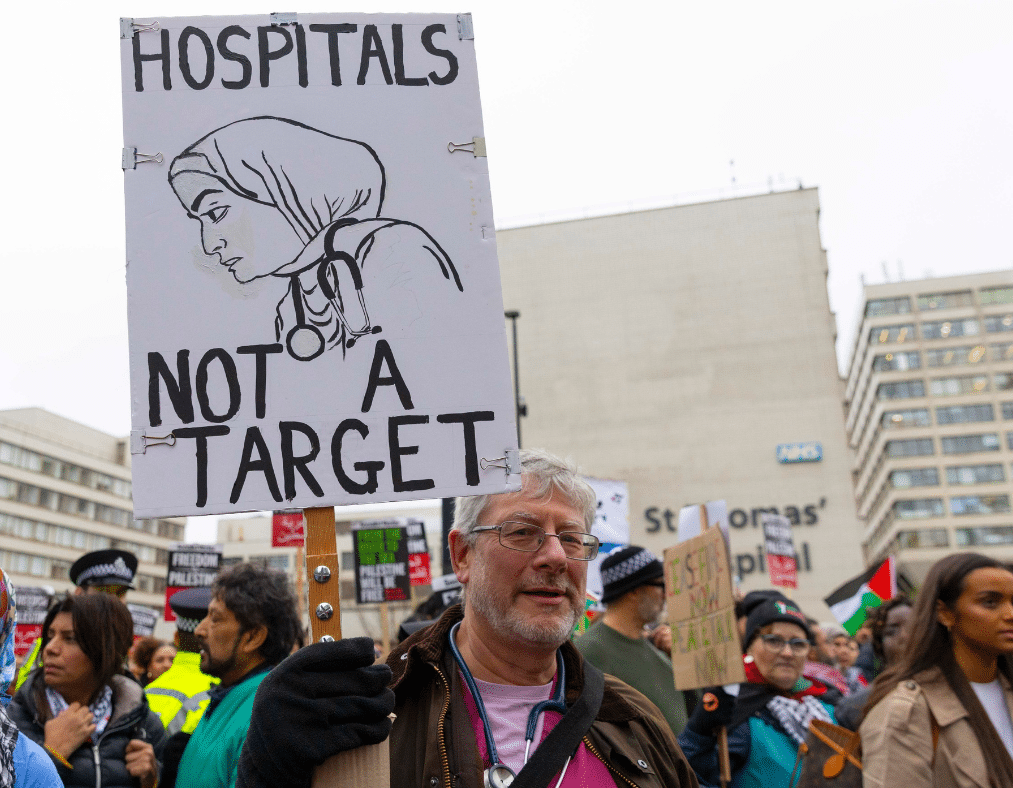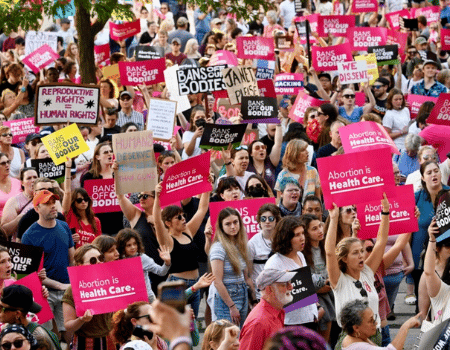Recent cuts to Official Development Assistance (ODA) are triggering a silent emergency—one that disproportionately impacts the women who hold up health systems across the globe. According to the World Health Organization (WHO), health ODA is projected to decline by as much as 40%, a shift with grave implications for countries already struggling to build and retain a resilient health workforce.These reductions directly threaten progress on the commitments made by Member States in WHA78.16, the resolution on health workforce and health systems financing adopted at the 78th World Health Assembly.
This landmark resolution—led by WHO and strongly supported by Nigeria—calls for urgent, sustained investment in the health workforce as a core pillar of health systems. It emphasizes the importance of domestic resource mobilization, country ownership, and gender-responsive investments, particularly in primary health care and community-based services. WHA78.16 affirms that resilient health systems require not only financial stability but also a rights-based approach that centers the wellbeing and leadership of women in health.
Crucially, both WHA 78.16 and the newly adopted resolution on health financing underscore that the achievement of Universal Health Coverage (UHC) is not possible without investing in the people—particularly women—who deliver care. Without adequate, sustainable funding for the health workforce, and without policies that prioritize gender equity and decent work, the foundational vision of UHC—health for all, without financial hardship—will remain out of reach.
Complementing WHA 78.16, Member States also adopted a Nigeria-sponsored resolution on health financing, reinforcing the call for greater public investment to accelerate UHC. The resolution urges governments to increase domestic spending on health, echoing the 2019 UN General Assembly call for at least 1% of GDP to be allocated to primary health care. It identifies potential fiscal levers—such as increased taxes on tobacco, sugar, and alcohol—that can both improve public health and generate additional revenues.
Importantly, the resolution encourages countries to invest in affordable, evidence-based essential health benefit packages, developed through inclusive and transparent national processes. This underscores the need to ensure that health systems are not only well-resourced but also equitable, accountable, and aligned with population needs.
The Assembly also marked a historic step forward in equity by recognizing—for the first time—rare and neglected skin diseases as global public health priorities, further widening the lens on inclusion in global health policy.
Yet despite these powerful resolutions and the momentum they represent, the harsh reality on the ground tells a different story. In Togo, Nigeria, Malawi, Zimbabwe, and many other countries, women health professionals are bearing the brunt of funding shortfalls. They are facing job losses, stalled careers, and the collapse of community-based care systems that once relied on consistent international support. Entire programs are being scaled back or shut down entirely—silencing voices, reducing access, and setting back progress toward gender equity, health equity, and the broader UHC agenda.
These are not just numbers. They are midwives without tools, researchers without funding, doctors working without pay, and entire communities left without care.
The testimonies that follow come from women across Africa, Asia, and beyond—those who are living the consequences of shrinking funding and systemic neglect. Their stories highlight both the fragility of the progress made and the extraordinary resilience of women leaders who continue to advocate for dignity, justice, and inclusion in global health.
As WHA78.16 so powerfully reminds us: health workforce investments are not only technical—they are political and moral imperatives. The achievement of Universal Health Coverage depends on them. Every budget cut has a face. And every missed investment is a lost opportunity to build a stronger, fairer, and more equitable global health system.
Togo
“In Togo, women health professionals are facing a wave of challenges brought on by cuts to Official Development Assistance (ODA). Community programs supporting reproductive health, maternal care, and education for girls are being scaled back or shut down. Health workers are losing their jobs, forced into unpaid roles, or denied training opportunities.
Partner organizations that previously benefited from international funding have had to scale down or stop their activities. This has led to cancellation of awareness-raising sessions, discontinuation of free contraception programs, and decreased funding for training of midwives and community health workers.
Several colleagues involved in local NGOs or co-funded projects have lost their jobs or been forced to volunteer due to lack of financial support.
I am working to launch an integrated women’s health center. However, access to funding, especially for start-up support and training, is becoming increasingly difficult. Available funds are often redirected toward other priorities, even as community needs grow.
These shifts are undermining efforts to advance women’s rights, health, leadership, and economic empowerment. Every budget cut has a face, often a woman’s, and carries profound human consequences.”
— Gynaecologist and Obstetrician, Togo
“In my role as a health facility director in Togo, I’ve witnessed first-hand how recent cuts in Official Development Assistance (ODA) are quietly but deeply affecting women in the health workforce.
Many community health programs led by women, including maternal health outreach, adolescent girls’ education, and reproductive health sensitization, have been scaled down or stopped altogether due to funding gaps. Several of the female contract staff who were part of these initiatives have lost their jobs or seen their hours cut, with no alternative support systems in place. This instability has had a direct impact on their mental health, income security, and leadership progression. Some were in line for supervisory roles, but the discontinuation of their contracts stalled their growth and shattered their confidence.
At the institutional level, budget reallocations have prioritized infrastructure over capacity building and wellness programs, often side-lining gender-focused leadership training. As a result, women’s voices in decision-making spaces are shrinking again after years of progress.
These changes are not just financial, they’re systemic setbacks. We urgently need to protect the gains made in women’s leadership and ensure that future funding models don’t erase the efforts of those who carry the backbone of our health systems.”
— Medical Doctor, Togo
Nigeria
“Until the abrupt stop-work order halted my organization’s funding, I held a senior leadership role that gave me purpose and stability. In an instant, I lost not just income, but also direction.
As a single mother and sole provider, the fallout was brutal. I had to relocate the same month my contract ended, with my savings drained and no financial cushion in sight. There were weeks I didn’t step outside, not by choice, but because the weight of not knowing what came next was simply too much. I sat in silence, watching rejection emails pile up, each one chipping away at my confidence. It has been a dark, grey stretch, where I’ve questioned my value, my progress, and even my identity.
This stillness wasn’t rest. It was grief. What hurts more is the silence, the invisible cost of donor decisions made far from the realities they disrupt. The ripple effect is profound: women leaders are stepping away, others are stretched thin just trying to hold on, and many are grieving the sudden loss of work we’ve poured years of ourselves into.
And yet, I’m holding on. Volunteering, consulting, building something new. Trying to stay anchored in purpose while navigating instability. But make no mistake: this moment is testing the very resilience we’ve built our careers upon.
For many women like me, it’s testing our mental health, our ability to lead, and our sense of safety in the systems we helped strengthen.
In moments like this, the role of communities like Women in Global Health becomes even more critical. Beyond advocacy, we need practical solidarity, emergency grants, mental health support, leadership transition fellowships, and platforms that help women remain visible and valued even when funding disappears. We need spaces to share, grieve, and rebuild together. Because the cost of these cuts cannot be silence, and the response cannot be invisibility. We’ve come too far for that.”
— Medical Doctor, Nigeria
“Due to recent cuts in development assistance, a community maternal health project I supported in rural Rivers State lost critical funding for training traditional birth attendants and providing delivery kits.
This setback reduced the frequency of outreaches and affected women’s access to safe delivery options.
It also limited leadership opportunities for young female health workers who were being mentored through the project. These cuts are silently reversing progress made in women’s health and leadership development in underserved communities. “
— Medical Doctor, Nigeria
“This is both a global and a local health challenge. One thing I have been able to do is to speak to stakeholders on the need to adapt to the change and advocate to our Government on the need to set priorities right.
In Nigeria, political offices take more than 50% of the total income of the Nation. We have witnessed how these politicians skyrocket contacts for themselves, accumulate so many material things including cars, houses, yachts, private jets, limited edition clothing, and designers at the expense of the people. I strongly believe that if there is a redirection and appropriate usage of funds, the cuts from ODA would not impact so much on Nigeria as it is now.”
— Public Health Physician, Nigeria
Malawi
“I was tasked with managing a highly technical project involving a diverse and complex consortium of partners. Despite my qualifications and track record, the senior management team, largely male began to express doubt in my ability to handle the project.
While no one explicitly mentioned my gender, the tone and content of the emails, the second-guessing, and the suggestion to bring back a former officer whose contract had ended made the underlying message clear: they didn’t believe a woman could lead such a high-stakes effort. The justification was that, they had identified gaps even without having evidence of my under performance. All my annual performance reviews indicated that I have been performing exceptionally well and beyond the organisation and donor’s expectations.
Eventually, I survived what was an unjust attempt at terminating my contract. That moment reinforced my belief in the importance of women holding space at the decision-making table and staying there, even when the room grows cold. At the same time, I’ve seen how cuts to Official Development Assistance (ODA) and shifts in global health funding are disproportionately affecting women in the workforce.
In my network, several women-led programs have been downsized or defunded, leading to job losses and reduced opportunities for mentorship, especially for young women professionals.
The ripple effects are real, from mental strain to loss of momentum in gender equity efforts. These shifts make it even harder for women to access leadership roles or sustain the gains we’ve fought so hard to make. Stories like mine and others within my professional circles show that while progress has been made, the foundation is still fragile and it is often women who bear the brunt when systems are shaken.”
— Program Manager, Malawi
“Recent cuts to Official Development Assistance (ODA)—particularly the withdrawal of USAID support—have had significant effects on women in the health workforce and the services they deliver. Previously, donor-supported programs paid nurses to work in neonatal units across district hospitals. These roles, often filled by young female nurses, provided experience, income, and development. With funding withdrawn, contracts ended, staffing decreased, and risks to newborns increased.
Mentorship coverage for maternal and newborn care has been severely reduced. Programs like Momentum Tiyeni enabled skilled female mentors to coach on-site. With fewer visits, support for junior staff—particularly women—is declining.
Clinical and neonatal death audits by senior specialists (many women) have become irregular, reducing efforts to prevent deaths and improve care. Cuts have also disrupted HIV services, especially PMTCT programs. With fewer trained staff, follow-up for HIV-positive mothers and babies has declined.
Many women health workers now face reduced opportunities and job insecurity.
These cuts undermine clinical outcomes and threaten years of progress in women’s leadership and health service delivery.”
— Clinical Training Manager, Malawi
“With the recent cuts in DA, I know of women who were economically independent and running their families become jobless and vulnerable to mental health challenges like depression as they figure out how to bounce back and regain their independency.”
— Health Advisor, Malawi
Zimbabwe
“I have had two consultancy assignments withdrawn and projects l have been working on stopped.
This has led me into financial distress and increased my dependence on my ex partner.
l feel frustrated because l have lost the progress l have made in my leadership journey and also lost my drive. However, this has given me time to reflect on the need to build resilience in the women health work force and psychosocial support structures.
l have participated in an Africa CDC Mental Health Leadership Course and l plan to use what l learnt to build capacity in mental health for working women.”
— Public Health Consultant, Zimbabwe
West and Central Africa
“Our research institution relies heavily on external partnerships to sustain our activities and provide continuous training opportunities.
Through an initiative led by WHO HRP, we established a regional research capacity-building hub, which included training programs aimed at strengthening institutional expertise. This initiative allowed me to pursue a doctoral program through a scholarship while also coordinating the project, ensuring that gender equity was a core principle in the selection and development of young researchers. As a result, we successfully increased female expertise within research teams across Francophone West Africa and parts of Central Africa. Unfortunately, due to budgetary constraints faced by our partners, we were unable to sustain this initiative.
The discontinuation of funding has significantly impacted training opportunities, mentorship programs, and institutional capacity-building efforts, limiting the ability of young researchers, especially women, to advance in their careers and contribute to gender-transformative health research.”
— Public Health Researcher, West and Central Africa Region
As a result of the ODA, many women especially those working in NGOs have lost their jobs while some are experiencing low pay but with the same amount of work. This imbalance causes stress and other psychological and emotional issues to women.Public Health Expert, Cameroon
With the limited financial resources of the association of women doctors, we have contributed to awareness raising, screening and training of women’s communities and we are satisfied with this.”
— Public Health Doctor, Ivory Coast
Sudan
“The workforce cuts are a mean of causing a surplus and a degradation of the workforce in order to serve the capitalist structure. More than a decade ago we used to question the funding apparatus and how it is not meeting its purpose in the global south.
Promoting women’s use of feminist methods should focus on putting health above militarisation and the harmful habits that the system is intended to support.
The goal should be to close the wealth gap between rich and poor nations and to assist them in creating green funds that can be used for development and health. The fundamental argument for raising people’s standard of living is to end the resource exploitation that is taking place in the southern part of the world and deal with all of the resources. Taxation and other financial factors should be carefully considered in order to support health and development.”
— Independent Consultant, Sudan
India
“Programs focused on women’s health being shut down with our partner organisation, and language of gender and sexuality muted”
— Thought leadership advisor and Program Manager, India
Colombia
“The course gave me the ability to better express in my networks and work spaces my position in relation to gender equality and the importance of making the issues visible in the public space. An example of them is to provide in my psychiatry classes the difference not only in income for health professionals between men and women but also in leadership positions at national and global level. It is necessary to be aware of the relationship in order to see it differently and transform it. Thank you for this valuable space.”
— Executive Director, Colombia
Canada
Chair, Excellencies, distinguished delegates,
I deliver this statement on behalf of the Medical Women’s International Association and the Alliance for Gender Equality and Universal Health Coverage—a coalition of over 165 civil society organizations representing 60 countries, advocating for gender-responsive health systems and universal access to sexual and reproductive health and rights (SRHR)—to the General Discussion for CPD58, April 2025.
As the Commission reflects on ensuring healthy lives and promoting well-being for all at all ages, we underscore the indivisibility of health and human rights. Universal Health Coverage will remain incomplete unless it intentionally addresses the specific needs of women, girls, adolescents, and marginalized communities across the life course.
We call on Member States to fulfill their commitments to gender equality and SRHR as enshrined in the 2030 Agenda and the Political Declaration on UHC. This includes:
Ensuring that essential health benefits packages fully integrate comprehensive SRHR services—from contraception and safe abortion to gender-based violence prevention, maternal health, and STI treatment;
Dismantling legal, financial, and social barriers—including gender discrimination, stigma, and punitive laws—that restrict access to quality health services;
Centering the voices and leadership of affected communities—particularly women, adolescents, LGBTQI+ people, Indigenous peoples, and those living in poverty—in the design, implementation, and accountability mechanisms of health systems.
We call for comprehensive sexuality education, digital inclusion, and intergenerational approaches, while emphasizing that the unpaid care burden on women and health workforce inequities must also be addressed to ensure sustainability.
UHC is not gender neutral. Health systems that ignore power, privilege, and patriarchy cannot deliver justice. We urge governments to invest in strong public health systems rooted in equity, rights, and solidarity—and to recognize that achieving health for all requires placing gender equality at the core.
— Medical Women’s International Association Statement Oral for CPD 58 April 2025
WHAT CAN YOU DO?
Help us raise awareness.
Share these stories on social media to spotlight the impact of global health cuts on women and demand policies and investments that center women’s leadership.
Share your story.
Are you witnessing the impact of these changes in your community or workplace?
We want to hear from you. Share your experience by emailing us at communications@womeningh.org and add your voice to this growing movement.